## Clinical Diagnostic Flowchart: Heart Failure (HF) Reasoning
### Overview
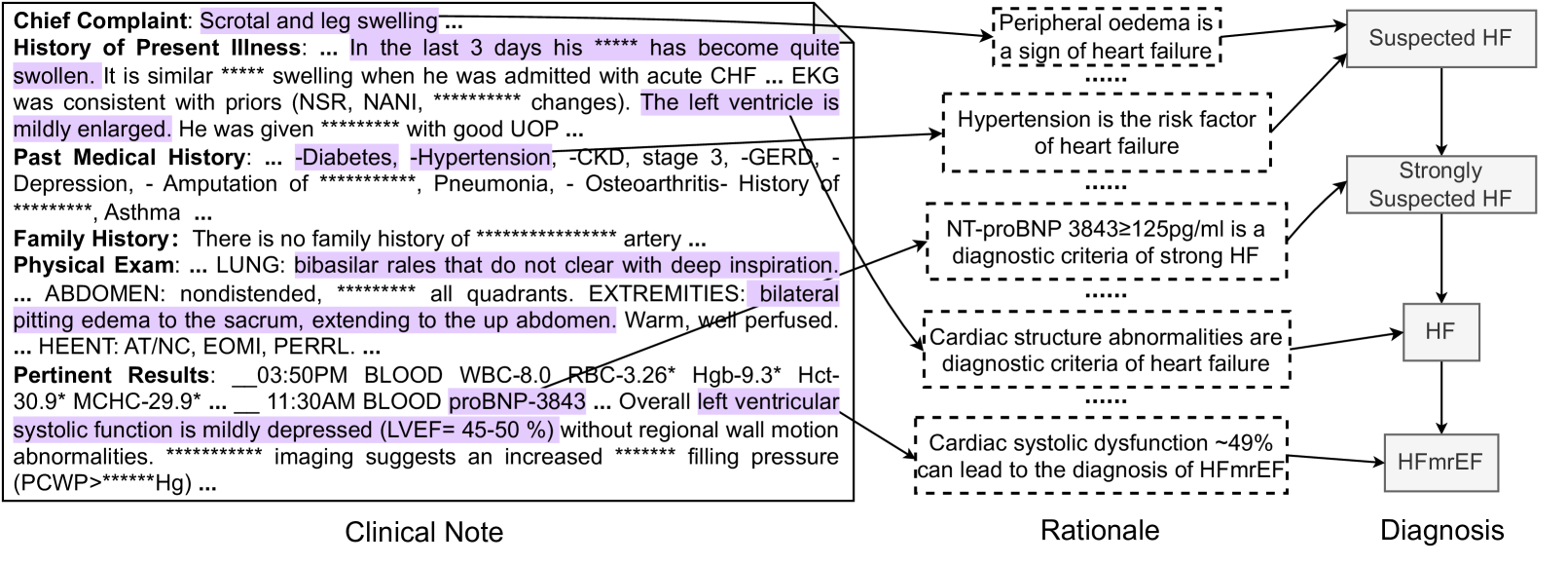
The image is a structured diagram illustrating the clinical reasoning process for diagnosing heart failure (HF), specifically HF with mildly reduced ejection fraction (HFmrEF). It visually maps information from a patient's clinical note to diagnostic rationales and final diagnostic conclusions. The diagram is divided into three vertical sections: **Clinical Note** (left), **Rationale** (center), and **Diagnosis** (right), connected by directional arrows.
### Components/Axes
The diagram has three primary components:
1. **Clinical Note (Left Panel):** A text block containing excerpts from a patient's medical record. Sections include Chief Complaint, History of Present Illness, Past Medical History, Family History, Physical Exam, and Pertinent Results. Specific phrases are highlighted in purple and connected via arrows to the Rationale section.
2. **Rationale (Center Panel):** A series of five vertically stacked, dashed-border boxes. Each box contains a medical statement that serves as a diagnostic criterion or risk factor for heart failure. Arrows from the Clinical Note point to these boxes, and arrows from these boxes point to the Diagnosis panel.
3. **Diagnosis (Right Panel):** A vertical flowchart of solid-bordered boxes showing a diagnostic progression: "Suspected HF" → "Strongly Suspected HF" → "HF" → "HFmrEF".
### Detailed Analysis
#### **Clinical Note Content (Transcribed with Redactions Noted)**
* **Chief Complaint:** Scrotal and leg swelling ...
* **History of Present Illness:** ... In the last 3 days his [REDACTED] has become quite swollen. It is similar [REDACTED] swelling when he was admitted with acute CHF ... EKG was consistent with priors (NSR, NANI, [REDACTED] changes). **The left ventricle is mildly enlarged.** He was given [REDACTED] with good UOP ...
* **Past Medical History:** ... -Diabetes, -Hypertension, -CKD, stage 3, -GERD, -Depression, - Amputation of [REDACTED], Pneumonia, - Osteoarthritis- History of [REDACTED], Asthma ...
* **Family History:** There is no family history of [REDACTED] artery ...
* **Physical Exam:** ... LUNG: **bibasilar rales that do not clear with deep inspiration.** ... ABDOMEN: nondistended, [REDACTED] all quadrants. EXTREMITIES: **bilateral pitting edema to the sacrum, extending to the up abdomen.** Warm, well perfused. ... HEENT: AT/NC, EOMI, PERRL. ...
* **Pertinent Results:** __03:50PM BLOOD WBC-8.0 RBC-3.26* Hgb-9.3* Hct-30.9* MCHC-29.9* ... __ 11:30AM BLOOD **proBNP-3843** ... **Overall left ventricular systolic function is mildly depressed (LVEF= 45-50 %) without regional wall motion abnormalities.** [REDACTED] imaging suggests an increased [REDACTED] filling pressure (PCWP>[REDACTED]Hg) ...
#### **Rationale Boxes (Content)**
1. **Top Box:** "Peripheral oedema is a sign of heart failure"
2. **Second Box:** "Hypertension is the risk factor of heart failure"
3. **Third Box:** "NT-proBNP 3843≥125pg/ml is a diagnostic criteria of strong HF"
4. **Fourth Box:** "Cardiac structure abnormalities are diagnostic criteria of heart failure"
5. **Bottom Box:** "Cardiac systolic dysfunction ~49% can lead to the diagnosis of HFmrEF"
#### **Diagnosis Flow**
The flowchart progresses sequentially downward:
1. **Suspected HF** (connected from Rationale boxes 1 & 2)
2. **Strongly Suspected HF** (connected from Rationale box 3)
3. **HF** (connected from Rationale box 4)
4. **HFmrEF** (connected from Rationale box 5)
### Key Observations
* **Evidence Linkage:** Purple highlights in the Clinical Note are directly linked to specific diagnostic rationales. For example, "bilateral pitting edema" links to "Peripheral oedema...", and "proBNP-3843" links to the NT-proBNP criterion.
* **Diagnostic Thresholds:** The rationale explicitly states a diagnostic threshold: NT-proBNP ≥125 pg/ml indicates "strong HF." The patient's value of 3843 far exceeds this.
* **Specific Diagnosis:** The final diagnosis is **HFmrEF**, which is defined by the rationale as associated with "Cardiac systolic dysfunction ~49%." This aligns with the clinical note's finding of "LVEF= 45-50 %."
* **Redactions:** Multiple terms are redacted with asterisks, likely to protect patient privacy or proprietary information. The redactions occur in the history, physical exam, and imaging results sections.
### Interpretation
This diagram is a visual representation of **clinical diagnostic reasoning**. It demonstrates how a clinician synthesizes disparate pieces of information from a patient's record—symptoms (edema), history (hypertension), lab work (elevated NT-proBNP), imaging (mildly enlarged left ventricle), and functional assessment (mildly depressed LVEF)—to arrive at a specific diagnosis.
The flowchart illustrates a **hierarchical and cumulative diagnostic process**:
1. Initial suspicion is raised by common signs and risk factors.
2. Suspicion is strengthened by a highly specific biomarker (NT-proBNP).
3. A general diagnosis of heart failure is confirmed by evidence of structural abnormality.
4. The diagnosis is further refined to a specific subtype (HFmrEF) based on the quantified level of systolic dysfunction.
The diagram emphasizes that the diagnosis of HFmrEF is not based on a single finding but on the convergence of multiple criteria. The patient's LVEF of 45-50% places them in the "mildly reduced" category, distinguishing it from HF with reduced ejection fraction (HFrEF) or preserved ejection fraction (HFpEF). The presence of elevated filling pressures (PCWP) further supports the diagnosis of heart failure.