TECHNICAL ASSET FINGERPRINT
f1da4250e621dfc2f487416c
Click to view fullscreen

Press ESC or click to close
FOUND IN PAPERS
EXPERT: gemini-2.0-flash VERSION 1
RUNTIME: nugit/gemini/gemini-2.0-flash
INTEL_VERIFIED
## Clinical Diagnosis Diagram: GERD vs. Suspected PBC
### Overview
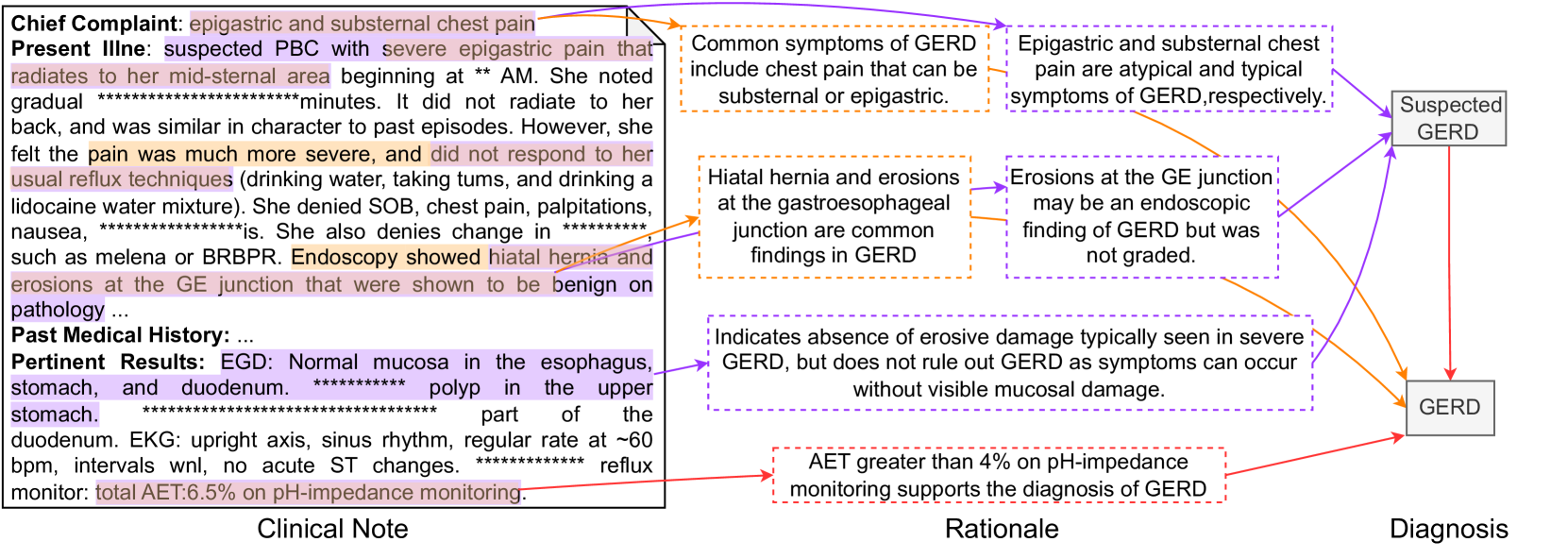
The image presents a clinical diagnostic diagram that differentiates between suspected Primary Biliary Cholangitis (PBC) and Gastroesophageal Reflux Disease (GERD). It connects clinical notes, rationale, and diagnosis through a series of statements and arrows, illustrating the thought process behind diagnosing GERD.
### Components/Axes
* **Clinical Note:** Contains patient's chief complaint, present illness, past medical history, and pertinent results from examinations.
* **Rationale:** Provides supporting statements and common findings related to GERD.
* **Diagnosis:** Indicates the final diagnosis of GERD.
* **Nodes:**
* "Suspected GERD" - A preliminary diagnostic consideration.
* "GERD" - The final diagnosis.
* **Connectors:** Arrows linking clinical findings to rationale and ultimately to the diagnosis.
* **Color Coding:**
* Purple arrows connect clinical findings to the "Suspected GERD" node.
* Orange arrows connect clinical findings and rationale to the "GERD" node.
* Red arrows connect specific clinical results to the "GERD" node.
### Detailed Analysis or Content Details
**Clinical Note (Left Side):**
* **Chief Complaint:** epigastric and substernal chest pain
* **Present Illness:** suspected PBC with severe epigastric pain that radiates to her mid-sternal area beginning at \*\* AM. She noted gradual \*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\*\u0000.000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000000
DECODING INTELLIGENCE...
EXPERT: gemma-3-27b-it-free VERSION 1
RUNTIME: google-free/gemma-3-27b-it
INTEL_VERIFIED
\n
## Flowchart: GERD Diagnostic Pathway
### Overview
This image presents a flowchart illustrating the diagnostic pathway for suspected Gastroesophageal Reflux Disease (GERD). It links clinical notes, rationale, and diagnosis, outlining the process from initial complaint to final diagnosis. The flowchart uses boxes to represent stages and arrows to indicate the flow of information.
### Components/Axes
The flowchart is divided into three main sections: "Clinical Note" (left), "Rationale" (center), and "Diagnosis" (right). Each section contains text boxes with information. Arrows connect these boxes, indicating the progression of the diagnostic process.
### Detailed Analysis or Content Details
**Clinical Note:**
* **Chief Complaint:** epigastric and substernal chest pain
* **Present Illness:** suspected PBC with severe epigastric pain that radiates to her mid-sternal area beginning at approximately 2 AM. She noted gradual pain over ~minutes. It did not radiate to her back, and was similar in character to past episodes. However, she felt the pain was much more severe, and did not respond to her usual reflux techniques (drinking water, taking turns, and drinking a lidocaine water mixture). She denied SOB, chest pain, palpitations, nausea, and changes in bowel habits such as melena or BRBPR. Endoscopy showed hiatal hernia and erosions at the GE junction that were shown to be benign on pathology.
* **Past Medical History:** ...
* **Pertinent Results:** EGD: Normal mucosa in the esophagus, stomach, and duodenum. Polyp in the upper stomach. Part of the duodenum. EKG: upright axis, sinus rhythm, regular rate at ~60 bpm, intervals w/n, no acute ST changes. Reflux monitor: total AET 6.5% on pH-impedance monitoring.
**Rationale:**
* Common symptoms of GERD include chest pain that can be substernal or epigastric.
* Epigastric and substernal chest pain are atypical and typical symptoms of GERD respectively.
* Hiatal hernia and erosions at the gastroesophageal junction are common findings in GERD.
* Erosions at the GE junction may be an endoscopic finding of GERD but was not graded.
* Indicates absence of erosive damage typically seen in severe GERD, but does not rule out GERD as symptoms can occur without visible mucosal damage.
* AET greater than 4% on pH-impedance monitoring supports the diagnosis of GERD.
**Diagnosis:**
* Suspected GERD (initial stage)
* GERD (final diagnosis)
The arrows indicate the following flow:
1. Clinical Note -> Rationale (Common Symptoms) -> Suspected GERD
2. Clinical Note -> Rationale (Hiatal Hernia/Erosions) -> Suspected GERD
3. Clinical Note -> Rationale (Erosions at GE Junction) -> Suspected GERD
4. Clinical Note -> Rationale (Absence of Erosive Damage) -> Suspected GERD
5. Clinical Note -> Rationale (AET > 4%) -> GERD
### Key Observations
The flowchart highlights that GERD diagnosis isn't solely based on the presence of erosions. Atypical symptoms, hiatal hernia, and pH-impedance monitoring results (AET > 4%) play a crucial role. The progression from "Suspected GERD" to "GERD" is dependent on the rationale provided.
### Interpretation
This flowchart demonstrates a clinical decision-making process for GERD. It emphasizes that GERD can be diagnosed even in the absence of significant erosive damage, relying on a combination of symptom presentation, endoscopic findings (like hiatal hernia), and physiological testing (pH-impedance monitoring). The AET value of 6.5% (from the clinical note) is a key factor supporting the final diagnosis of GERD. The flowchart is a simplified representation of a complex diagnostic process, but it effectively illustrates the key considerations for clinicians. The use of "approximately" (~), and "within" (w/n) indicates uncertainty in the values. The repeated asterisks (********) likely represent redacted patient information.
DECODING INTELLIGENCE...
EXPERT: healer-alpha-free VERSION 1
RUNTIME: free/openrouter/healer-alpha
INTEL_VERIFIED
## Medical Case Analysis Diagram: GERD Diagnostic Pathway
### Overview
This image is a structured medical case analysis diagram that traces the diagnostic reasoning for a patient presenting with chest pain. It visually maps specific findings from a clinical note to their medical rationale, culminating in a diagnosis of GERD (Gastroesophageal Reflux Disease). The diagram is organized into three vertical columns: **Clinical Note** (left), **Rationale** (center), and **Diagnosis** (right). Colored highlights and arrows create explicit links between patient data, medical reasoning, and diagnostic conclusions.
### Components/Axes
The diagram is segmented into three primary regions:
1. **Clinical Note (Left Column):** Contains transcribed excerpts from a patient's medical record.
* **Sections:** Chief Complaint, Present Illness, Past Medical History (truncated), Pertinent Results.
* **Highlighted Text Segments:** Text is highlighted in three colors, each corresponding to a different diagnostic thread:
* **Orange:** Symptoms and findings commonly associated with GERD.
* **Purple:** Atypical symptoms or findings that require specific interpretation.
* **Red:** Objective test results that provide strong diagnostic evidence.
* **Redacted Information:** Several sections of text are obscured with asterisks (`***`), indicating omitted or irrelevant details for this specific analysis.
2. **Rationale (Center Column):** Contains explanatory text boxes that interpret the highlighted clinical findings.
* **Box Style:** Each rationale is enclosed in a dashed border, with the border color matching the highlight color from the Clinical Note (orange, purple, or red).
* **Content:** Each box provides a medical fact or interpretation that connects a specific clinical finding to the diagnosis of GERD.
3. **Diagnosis (Right Column):** Contains the final diagnostic conclusions.
* **Boxes:** Two gray boxes labeled "Suspected GERD" and "GERD".
* **Flow:** Arrows indicate the progression from suspicion to a more definitive diagnosis based on the aggregated evidence.
**Spatial Grounding & Connections:**
* **Arrows:** Colored arrows (orange, purple, red) originate from highlighted text in the Clinical Note, pass through or connect to corresponding rationale boxes, and terminate at the diagnosis boxes.
* **Legend/Color Code:** The color of the highlight, rationale box border, and connecting arrow are consistent for each diagnostic thread:
* **Orange Thread:** Links common GERD symptoms (chest pain) and common endoscopic findings (hiatal hernia, erosions) to both "Suspected GERD" and "GERD".
* **Purple Thread:** Links atypical symptom descriptions and the *absence* of severe erosive damage to "Suspected GERD" and "GERD", with a rationale clarifying that this does not rule out GERD.
* **Red Thread:** Links the objective pH-impedance monitoring result directly to the "GERD" diagnosis box.
### Detailed Analysis
**Clinical Note Transcription (with highlights noted):**
* **Chief Complaint:** `epigastric and substernal chest pain` (Highlighted in **Orange**)
* **Present Illness:** `suspected PBC with severe epigastric pain that radiates to her mid-sternal area` (Highlighted in **Purple**). The note describes pain not responding to usual reflux techniques. It also states: `Endoscopy showed hiatal hernia and erosions at the GE junction that were shown to be benign on pathology` (Highlighted in **Orange**).
* **Pertinent Results:**
* `EGD: Normal mucosa in the esophagus, stomach, and duodenum. ********** polyp in the upper stomach. *************** part of the duodenum.` (Highlighted in **Purple**)
* `EKG: upright axis, sinus rhythm, regular rate at ~60 bpm, intervals wnl, no acute ST changes. *********** reflux monitor: total AET:6.5% on pH-impedance monitoring.` (Highlighted in **Red**)
**Rationale Boxes (Transcribed):**
1. **(Orange Border):** `Common symptoms of GERD include chest pain that can be substernal or epigastric.`
2. **(Orange Border):** `Hiatal hernia and erosions at the gastroesophageal junction are common findings in GERD`
3. **(Purple Border):** `Epigastric and substernal chest pain are atypical and typical symptoms of GERD, respectively.`
4. **(Purple Border):** `Erosions at the GE junction may be an endoscopic finding of GERD but was not graded.`
5. **(Purple Border):** `Indicates absence of erosive damage typically seen in severe GERD, but does not rule out GERD as symptoms can occur without visible mucosal damage.`
6. **(Red Border):** `AET greater than 4% on pH-impedance monitoring supports the diagnosis of GERD`
**Diagnosis Flow:**
* Arrows from the orange and purple rationale threads converge on the **"Suspected GERD"** box.
* All three threads (orange, purple, and red) have arrows pointing to the final **"GERD"** box, indicating a conclusive diagnosis based on the totality of evidence.
### Key Observations
1. **Multi-Evidence Diagnosis:** The diagnosis is not based on a single finding but on a confluence of symptomatic, endoscopic, and objective physiological data.
2. **Handling of Contradictory Evidence:** The diagram explicitly addresses a potential contradiction: the endoscopy showed only mild findings (hiatal hernia, non-graded erosions) and "normal mucosa," which might suggest severe erosive GERD is absent. The purple rationale box clarifies that this absence does not rule out GERD.
3. **Objective vs. Subjective Data:** The strongest, most objective piece of evidence (pH-impedance monitoring with AET 6.5%) is highlighted in red and has a direct, unambiguous arrow to the final "GERD" diagnosis.
4. **Use of Redaction:** The use of `***` focuses the analysis on the medically pertinent information, stripping away irrelevant history or details for this specific diagnostic question.
### Interpretation
This diagram serves as a visual clinical reasoning tool. It demonstrates how a physician synthesizes disparate pieces of patient data to arrive at a diagnosis.
* **What the Data Suggests:** The patient's presentation of epigastric/substernal pain, combined with common endoscopic findings (hiatal hernia) and, most importantly, an Acid Exposure Time (AET) of 6.5% (above the 4% diagnostic threshold), strongly supports a diagnosis of GERD. The diagram successfully argues that even in the absence of severe erosive damage on endoscopy, the symptomatic and pH-impedance evidence is sufficient.
* **Relationship Between Elements:** The arrows create a clear "if-then" logic chain. *If* a patient has symptom X (orange), *then* it is a common symptom of GERD. *If* a test shows result Y (red), *then* it supports the diagnosis. The rationale boxes provide the medical knowledge that justifies these logical links.
* **Notable Pattern:** The pathway highlights a modern diagnostic approach to GERD, which relies heavily on objective physiological testing (pH-impedance monitoring) to confirm or rule out the disease, especially when endoscopic findings are ambiguous or mild. The diagram effectively communicates that GERD is a clinical diagnosis supported by evidence, not solely defined by visible damage to the esophagus.
DECODING INTELLIGENCE...
EXPERT: nemotron-free VERSION 1
RUNTIME: free/nvidia/nemotron-nano-12b-v2-vl:free
INTEL_VERIFIED
# Technical Document Extraction: Clinical Note Flowchart
## Overview
The image is a flowchart diagram summarizing a clinical note for a patient with suspected Gastroesophageal Reflux Disease (GERD). The diagram is divided into three main sections: **Clinical Note**, **Rationale**, and **Diagnosis**, with color-coded arrows connecting symptoms, findings, and conclusions.
---
## Clinical Note Section
### Key Labels and Text
- **Chief Complaint**:
- "epigastric and substernal chest pain"
- **Present Illness**:
- "suspected PBC with severe epigastric pain that radiates to her mid-sternal area beginning at ** AM."
- "It did not radiate to her back, and was similar in character to past episodes."
- "She denied water, taking tums, and drinking a lidocaine water mixture."
- "She denied SOB, chest pain, palpitations, nausea, ******."
- "She also denies changes in ****** such as melena or BRBPR."
- "Endoscopy showed hiatal hernia and erosions at the GE junction that were shown to be benign on pathology..."
- **Past Medical History**:
- "..." (No details provided)
- **Pertinent Results**:
- "EGD: Normal mucosa in the esophagus, stomach, and duodenum. ****** polyp in the upper stomach, ****** of the duodenum."
- "EKG: upright axis, sinus rhythm, regular rate at ~60 bpm, intervals wnl, no acute ST changes. ****** reflux monitor: total AET:6.5% on pH-impedance monitoring."
### Highlighted Text (Key Findings)
- **Epigastric and substernal chest pain** (purple highlight)
- **Hiatal hernia and erosions at the GE junction** (orange highlight)
- **Normal mucosa in the esophagus, stomach, and duodenum** (blue highlight)
- **AET greater than 4% on pH-impedance monitoring** (red highlight)
---
## Rationale Section
### Key Labels and Text
- **Common symptoms of GERD**:
- "include chest pain that can be substernal or epigastric."
- **Hiatal hernia and erosions at the gastroesophageal junction**:
- "are common findings in GERD."
- **Absence of erosive damage**:
- "Indicates absence of erosive damage typically seen in severe GERD, but does not rule out GERD as symptoms can occur without visible mucosal damage."
- **AET >4% on pH-impedance monitoring**:
- "supports the diagnosis of GERD."
### Color-Coded Arrows
- **Purple arrows**: Link symptoms (e.g., epigastric/substernal chest pain) to GERD.
- **Orange arrows**: Connect findings (e.g., hiatal hernia, erosions) to GERD.
- **Red arrows**: Highlight diagnostic support (e.g., AET >4%).
---
## Diagnosis Section
### Key Labels and Text
- **Suspected GERD**:
- "Epigastric and substernal chest pain are atypical and typical symptoms of GERD, respectively."
- **Final Diagnosis**:
- "GERD" (confirmed via flowchart connections).
- "AET greater than 4% on pH-impedance monitoring supports the diagnosis of GERD."
---
## Diagram Components and Flow
1. **Clinical Note**:
- Contains patient history, symptoms, and test results.
- Highlighted text emphasizes critical findings (e.g., chest pain, hiatal hernia).
2. **Rationale**:
- Explains how symptoms and findings align with GERD.
- Uses color-coded arrows to map connections:
- Purple: Symptom → GERD
- Orange: Finding → GERD
- Red: Diagnostic support → GERD
3. **Diagnosis**:
- Concludes with "GERD" as the final diagnosis.
- Reinforces AET >4% as a key diagnostic criterion.
---
## Color Legend and Spatial Grounding
- **Legend**: Not explicitly labeled, but colors are used consistently:
- **Purple**: Symptoms (e.g., chest pain).
- **Orange**: Findings (e.g., hiatal hernia).
- **Red**: Diagnostic support (e.g., AET >4%).
- **Spatial Placement**:
- Clinical Note: Left side.
- Rationale: Middle.
- Diagnosis: Right side.
---
## Key Trends and Data Points
- **Symptoms**:
- Epigastric and substernal chest pain (atypical and typical GERD symptoms).
- **Findings**:
- Hiatal hernia and erosions at the GE junction (confirmed via endoscopy).
- **Test Results**:
- Normal mucosa in EGD but presence of a polyp in the upper stomach.
- EKG: Normal sinus rhythm, no acute ST changes.
- AET: 6.5% on pH-impedance monitoring (supports GERD diagnosis).
---
## Conclusion
The flowchart systematically links clinical symptoms, endoscopic findings, and diagnostic test results to confirm GERD. The use of color-coded arrows clarifies the reasoning process, emphasizing that while erosive damage is absent, other criteria (e.g., AET >4%) validate the diagnosis.
DECODING INTELLIGENCE...